Six months ago we launched our campaign – and today we are delighted to announce our first significant victory in our Fight4Treatment. The Health Service Journal (HSJ) had today reported that NHS England are to publish a policy that will allow patients with urgent need to get funding for Everolimus for those who’s health means they cannot wait for a national policy to emerge.
Exclusive: NHS England proposes new rare condition
drug access rules
21
May, 2015 | By Shaun
Lintern
NHS
England is set to publish new guidance, described by charities as ‘life
saving’, on access to licensed drugs for patients with rare conditions and in
‘critical need’, HSJ has learned.
The
proposed new policy, which is expected to be signed off by NHS England chief
executive Simon Stevens, follows allegations by some medical specialists that a
delay to changing existing processes has meant patients with critical need
“have [had] no hope of access to funding” despite facing a “high risk of preventable death”, and led to avoidable deaths.
NHS
England has contested this.
However, HSJ has
learned NHS England is preparing new standard operating procedures for the
consideration of critically urgent cases where there is no established policy,
with the intention of publishing it next week.
An
email sent last week to NHS England’s patient and public voice assurance group
by Fraser Woodward, head of engagement and partnerships for specialised
commissioning for NHS England and seen by HSJ, said a new draft
standard operating procedure for dealing with critically urgent cases was being
developed.
Mr
Woodward said the new policy would require “sign off from Simon Stevens” but
that once published, “would update and supersede” a circular on access for
patients in urgent need, which was published in 2013.
The
2013 circular highlighted a problem for patients with rare conditions which had
arisen from the Health Act 2012 commissioning restructure, and put in place
what it said was an interim access process to deal with this, which it said
would expire in March last year. It warned that when primary care trusts were
scrapped, the number of patients applying for an individual funding request for
interim access to drugs to treat rare conditions was aggregated nationally.
This meant there were too many to be considered exceptional, which the policy
limited to no more than five a year.
In
recent months, several charities have told HSJ they believed
this interim policy had expired in March 2014 as planned, and that this had led
to patients in urgent need to being able to access drugs. NHS England has
insisted that, despite the stated expiry date, the interim policy remains in
place and was being used.
However,
the Tuberous Sclerosis Association, which represents patients with tuberous
sclerosis complex, told HSJit believed the replacement policy which
has now been proposed could be a “life saver” for these individuals, compared
to the current situation.
Association
chief executive Jayne Spink said it could be “a life saver for the adults and
children with critical need and TSC”. She added: “We will be testing the policy
on our 30-plus critical need patients. What we then need NHS England to do is
to get on with developing the policy for non-urgent cases.”
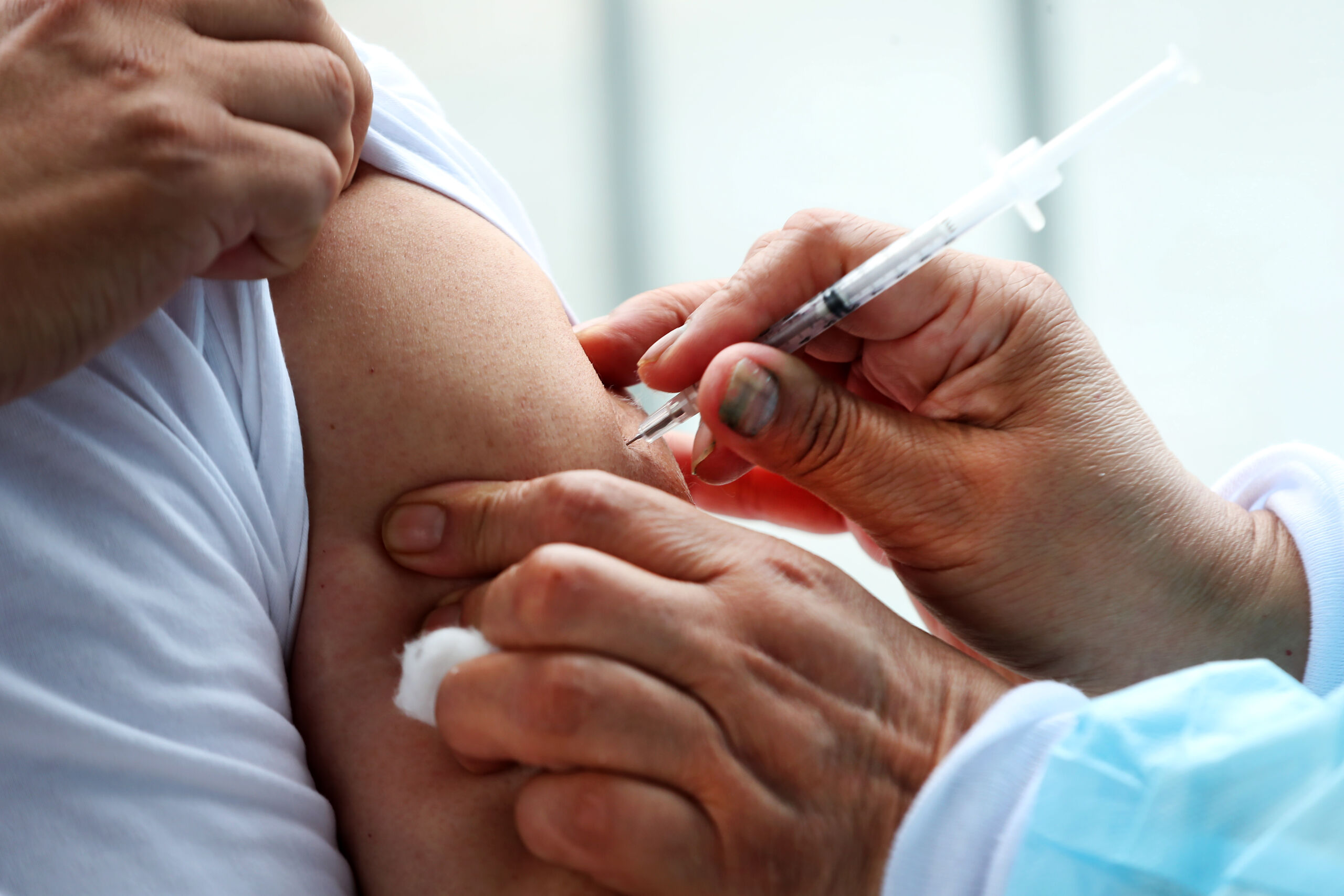
TSC
can be treated by the drug everolimus, which was licensed for use in TSC
patients in 2012, but has not been considered by the National Institute for
Health and Care Excellence.
Ms
Spink said the proposal should also help patients in critical need with other
rare conditions. HSJ has previously covered concerns about
those with Morquio syndrome, and Duchenne muscular dystrophy.
NHS
England has insisted there is already a process in place to consider cases such
as these as “individual funding requests”. However, it said an example in
February had seen a request patient denied treatment, despite a “massive life
threatening bleed”, because it was “representative of a group of patients who
have a similar condition and are at the same stage of that condition and who
could potentially all request the same treatment”. This meant, it said: “In
this circumstance, this is a request for a service development and is not
appropriate for consideration as an IFR.”
NHS
England also said an interim policy remained in place for access for critically
urgent cases. During 2013-14 and 2014-15 there were 46 applications by doctors
to treat TSC patients with everolimus, and 15 approved.
In
relation to the new guidance for critically urgent cases, an NHS England
spokesman said: “We are currently refreshing the standard operating procedure for
considering these cases, as well as producing information on it for patients
and clinicians, and will be publishing these shortly.”
The article is available to view online here